|
Dr. David Musnick, MD Functional Medicine Doctor Sport Medicine & Orthopedics |
Diagnosis Misses | Symptoms | Pathophysiology & Treatment
When a person experiences a head injury, they may go to the emergency room where a doctor will often order a CAT scan to look for evidence of a brain bleed. More often than not the CAT scan will show no acute bleed. The person is sent home with a list of symptoms to look for to help them identify post-concussion syndrome. They generally don’t receive treatment suggestions that will address the physiology of what is going on in their brain, just a suggestion that rest and time will heal their injury.
The problem is that this conventional approach often misses secondary brain injuries that can occur in specific areas of the brain. Left untreated, this damage may lead to diminished brain reserves, headaches, memory loss and other issues in the areas in the brain that were affected.
After years of treating various head injuries and observing the deficiencies of the conventional method, I developed a functional medicine approach that addresses the pathophysiology of brain injuries. In other words, a way to identify what is happening in the brain as a result of the injury. But more specifically, a way to identify and treat the areas of the brain that may have been neglected in a traditional evaluation.
The objective of this article is to increase the awareness of these options, so you can share with your physician, improve treatment effectiveness, and minimize the incidents of an untreated secondary brain injury.
Can I Have mTBI and Not Know It?
 In the early days it was my joint interest in sports medicine and holistic medicine that led me to study concussions and brain injuries. But, while NFL concussions might take center stage in the media, there are many ways a person can develop a concussion or other mild head trauma.
In the early days it was my joint interest in sports medicine and holistic medicine that led me to study concussions and brain injuries. But, while NFL concussions might take center stage in the media, there are many ways a person can develop a concussion or other mild head trauma.
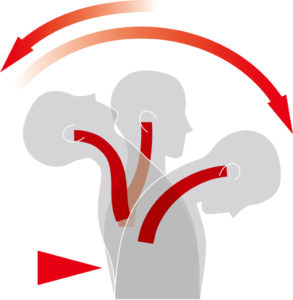
Often head injuries are a result of hitting your head during an accident or a fall. What many people don’t realize, is that you can also get a concussion without hitting your head. If an accident causes extreme head movement (such as your head rocking back and forth when your car is rear-ended) your brain can slam into your skull from inside your head.
If asked, “did you hit your head,” the patient will say no, but that doesn’t mean they didn’t get a concussion from the accident. Becoming aware of potential brain-damaging events and sharing your concerns during the initial assessment is extremely important. This will allow any potential brain injury to be properly evaluated and treated.
mTBI & Secondary Brain Injury Symptoms
The Timeline Challenge
Primary concussion symptoms can include headache, nausea, blurry vision, fatigue and depression. A patient can also experience extreme fatigue and insomnia. These symptoms will typically resolve in 4-6 weeks.
Secondary symptoms can start to appear up to a week after the injury and are often related to the specific areas of the brain that were injured. These secondary symptoms can include:
- Problems finding words
- Short term memory loss
- Lack of focus or ability to concentrate
- Hard to understand words
- Impaired executive function – difficulty multitasking
- “Brain fog” or slow thinking
- Sensitivity to light or sound (from neurons reaching their threshold, so they fire too easily)
Depending on how quickly a loss of neurons happens in the brain, some of these symptoms may show up two weeks after the injury. This can make it difficult to connect the dots and link some of these symptoms to the head trauma.
With children, there are additional challenges as they are not always aware of their symptoms or able to communicate how they feel. As a result, it can take parents longer to realize something is wrong.
Common Pitfalls of the Conventional Approach
In addition to the challenges in the discovery process, where some symptoms are overlooked and may not be associated to the actual injury, there often other challenges that arise after symptoms are identified.
Mapping the symptoms to the affected areas in the brain
Once symptoms are discovered, it is essential to connect them to the specific areas of the brain that may be affected. Standard MRI and CAT scans are usually not very helpful in capturing the damaged areas of the brain, so it is important to work with a clinician that understands the physiology of the brain.
Time is crucial
Often when these issues are not captured and addressed right away, the damage is quietly occurring behind the scenes and the brain may continue to deteriorate. Treatments are most effective when they start as early as possible.
Identifying the related symptoms
To avoid these common consequences of head injury and manage the symptoms as soon as possible:
- Work with a physician that understands the physiology of the brain, ideally someone who is specialized in functional neurology.
- Share all the different symptoms you experience for up to 2 weeks after the injury, to identify those that may be related to the head trauma.
The Functional Medicine Approach to mTBI
The pathophysiology of a head injury

Listed below are some of the key pathophysiological mechanisms and treatment targets after a head injury.
As I have mentioned earlier, the objective of this information is to increase the awareness of these potential issues, so you can share with your doctor to make sure they are properly evaluated and addressed.
1 – Brain Hypoxia
Reduced supply of oxygen to the brain
Treatment options to start as soon as possible:
- Hyperbaric oxygen therapy (HBOT):
Works by improving oxygenation in problematic tissues that may not be getting enough oxygen. This treatment has been used for years for wound care and diving injuries. Several studies have suggested that HBOT may be effective for patients with mild traumatic brain injury by increasing oxygenation in the brain. - Nitric oxide supplements:
Arginine and citrulline can help improve nitric oxide in the brain. Nitric oxide acts as an important neurotransmitter in the brain and plays an important role in connecting blood vessels and neurons. - Vinpocetine & ginkgo biloba:
Two dietary supplements that can also help to increase oxygen and blood flow in the brain.
2 – Excessive Excitotoxicity
Rapid influx of calcium via NMDA receptors that can lead to damage and death of cells.
Treatments options:
- Avoid foods or drinks with monosodium glutamate (MSG) or aspartame.
- Stop all calcium supplements during the first few weeks
- Magnesium I-threonate:
A type of magnesium shown to increase brain levels of magnesium, which can help to limit excitotoxicity by acting as a natural NMDA receptor blocker. - Taurine
An amino acid that can be extremely helpful during all stages of head injury, including providing protection against excitotoxicity. - N-Acetyl Cysteine (NAC):
An amino acid that may also play a role in decreasing excitotoxicity. It also helps replenish glutathione, an important antioxidant in the body.
3 – Mitochondrial Damage
Low energy, fatigue
 Mitochondria are the energy producing areas of the cells. As a result of the injury, the mitochondria can have difficulty making energy, especially 5-7 days after the incident. So you may feel low in energy, tired after cognitive activities, or experience general fatigue.
Mitochondria are the energy producing areas of the cells. As a result of the injury, the mitochondria can have difficulty making energy, especially 5-7 days after the incident. So you may feel low in energy, tired after cognitive activities, or experience general fatigue.
Treatments options focus on targeted supplements with specific nutrients the mitochondria need to make energy:
- Methylated B vitamins (the active forms of the B vitamins)
- CoQ10
- Glutathione
- DHA Omega 3
- NAD+ & Resveratrol (for cases of high brain fatigue)
4 – Neural Inflammation in the Brain
Brain Inflammation
Sometimes as a result of the head injury, the microglial cells in the brain get injured and become inflamed. The microglial cells play a key role in many brain functions, including the production of necessary chemicals and trophic factors, which help to nourish the neurons and create new synaptic connections.
Treatment options focus on reducing the inflammation and nourishing the brain with a specific anti-inflammatory brain injury diet & supplements.
5 – Digestive Problems after Head Injury
The gut-brain axis
 All people who have previously suffered a head injury should be asked about digestive issues such as gas, bloating, constipation or diarrhea. It is common for a patient with a concussion to develop gastrointestinal tract dysfunction such as vagus nerve damage, slow motility, and changes in the gut microbiome.
All people who have previously suffered a head injury should be asked about digestive issues such as gas, bloating, constipation or diarrhea. It is common for a patient with a concussion to develop gastrointestinal tract dysfunction such as vagus nerve damage, slow motility, and changes in the gut microbiome.
This can become a serious issue, as the injury to the brain may cause autoimmunity to the gut lining, brain tissue or the blood brain barrier. For this reason, if there are any gastrointestinal tract symptoms, I recommend having antibody testing done for the intestine and the blood brain barrier to determine if this is indeed an issue.
Treatment options may vary depending on the damage to the GI tract and typically focus on a dietary protocol designed to reduce gut inflammation and restore gut health.
Additional Treatment Options
In addition to the main pathophysiological mechanisms and treatment targets mentioned above, below are important therapy options and lifestyle consideration that can also support the healing process.
Exercise
 You might be surprised to know that aerobic exercise can actually help in treating head injuries. Cardiovascular exercise is shown to increase a protein called brain-derived neurotrophic factor (BDNF), which plays a key role in the repair process and the creation of new neurons and synaptic connections.
You might be surprised to know that aerobic exercise can actually help in treating head injuries. Cardiovascular exercise is shown to increase a protein called brain-derived neurotrophic factor (BDNF), which plays a key role in the repair process and the creation of new neurons and synaptic connections.
When the patient has enough energy, I highly recommend incorporating exercise. While the workout load should match the patient’s fitness level, the recommended intensity is 40 minutes of aerobic activity 4-5 days a week at 70-80% of the patient’s maximum heart rate. If you don’t have a heart rate monitor, this translates to exercise where it is challenging to carry on a conversation of more than a few words.
Get More Sleep
Sleep is incredibly important since a significant part of the brain healing occurs while we are sleeping. Ideally, you should sleep for 8 hours or more every night.
People often have neck injuries with their head injuries, so they are in pain. As a result of the pain they may not sleep well. In other cases, you may be experiencing emotional stress after the injury that can also cause sleeping problems.
Several studies show that as little as three days of poor sleep, we can already see an increase in inflammatory markers. If you experience sleeping problems after the injury, it is important to give it the proper attention. If necessary, you should work with your doctor on the different options to improve sleep.
Frequency specific microcurrent (FSM)
FSM is a treatment that delivers micro amperage currents in specific frequencies to various tissues in the body. It is a type of micro current that can treat inflammation in the brain, including the brain injury itself. In my practice, I have found the FSM treatment a safe and effective therapy option in cases of musculoskeletal and brain injuries.
Limit Electromagnetic Fields (EMFs) Exposure
While the general public usually doesn’t hear much about it, we already have enough information about the potential harmful effects of EMFs to the brain. I believe it’s a good idea to take precautions and decrease exposure after a head injury. This is important especially for children who are more sensitive to electromagnetic currents.
While it is usually not possible to completely avoid EMFs, here are some ways to reduce EMF exposure for you to consider. This is especially important at night, where the majority of the brain healing takes place:
- Do not hold your cell phone near the head
- Turn the WiFi routers off at night
- Turn off your cell phone at night or place it away from your bedroom
- Disable other WiFi smart devices
- Power off electric beds, smart beds, and electric blankets.
- Use a smart meter shield.
Summary
Concussion and mild traumatic brain injury are common, although are they are inadequately treated by the conventional medical approach. I believe that the functional medicine approach has the ability to significantly improve the efficacy of treatment and minimize the incidents of an untreated secondary brain injury. Use this information to educate yourself and share these options with your physician.
Read Next
The Brain Injury Diet: Best Foods & Supplements For mTBI and Concussions.