 |
Melissa Pyette, RDH, MS Integrative Nutrition Registered Dental Hygienist |
Link to disease | Leaky mouth | Warning signs | Diet | Dental care tips
In this post, you will learn about the connection between oral health and overall health, warning signs to watch for, and practical dietary and oral care tips to optimize your dental wellness.
What Happens in the Mouth, Doesn’t Stay in the Mouth
Our culture often holds a disconnected perception of how the mouth and body are linked. Oral health and wellness education can bridge this disconnect. The mouth is a major pathway that introduces either nutritious or toxic substances to your body. Fact, what we put in our mouth will enter our body. We are what we eat!
Nutritious food choices have one of the biggest single impacts on oral health. Your teeth and gums are living tissues that need ongoing nourishment just like the rest of the body. The mouth is not an isolated “organ”. It is deeply connected to the entire system. Poor oral health can affect the entire body and the issues within our body can affect our mouths. So, when we talk about health and wellness, we should always consider our oral health as an important part of the picture.
The Plot Thickens: Poor Oral Health & Chronic Disease

You may have heard the famous quote by Hippocrates, the father of medicine, “All disease begins in the gut.”
Indeed, the connection between our gut to our overall health and well-being has been extensively studied and accepted by the scientific community.
So, we know health begins in the gut, but the health of our gut, actually begins in our mouth! According to research, oral bacteria can spread through the body and affect the gut microbiome.[1]
In fact, mountains of studies support the connection between oral health and inflammatory diseases. Periodontal disease or gum infection is correlated with conditions such as diabetes, insulin resistance, rheumatoid arthritis, cardiovascular disease, stroke, adverse pregnancy outcomes, erectile dysfunction, and even Alzheimer’s disease.
So how does this happen?
The mouth is the gatekeeper to our entire digestive tract, which is part of our immune system. It is the first step of the digestive process. Just like the gut, the mouth has its own unique microbiome. When the mouth microbiome is balanced, the good bacteria protect us from pathogens and support healthy digestion. When dysbiosis or microbial imbalance occurs, the mouth can seed pathogens to other areas of our body, compromising our entire immune system.
Leaky Mouth & Gut Health
I often refer to microbial imbalance in the mouth as a leaky mouth. Just like imbalances in the gut, known as a leaky gut, allow unwanted substances to “leak” into circulation, the same thing happens when the bacteria in the mouth are comprised. Since the mouth is easier to examine it may be the first clinical area where chronic inflammation can be diagnosed.
Poor gut health, on the other hand, can also affect the mouth. It is thought that periodontal disease originates in the gut, even before becoming visible in the mouth. That’s why it is so important to heal an unhealthy gut and an unhealthy mouth as they continue influencing one another.
Warning Signs of Poor Oral Health

Say ah! The mouth is a mirror to your internal health. So, what do your tongue, teeth, lips, saliva, breath and gums reveal about your health?
Below are some of the more common yet overlooked symptoms of poor oral care that may be related to an underlying health issue. Keep in mind, these are not meant for you to self-diagnose, but to help you become more aware of the signs, so you can share with your doctor if relevant.
Too Little Saliva (Xerostomia)
A healthy flow of saliva helps wash away bad bacteria and also acts as a buffer to acid, which balances the pH levels in the mouth.
Digestion starts in the mouth and saliva plays a key role in the process by moistening the foods we eat. This helps create a bolus so foods can be easily swallowed.
Too little saliva, called xerostomia, compromises a person’s dietary intake, oral health, and in fact, may affect quality of life. If you have an unusual dry mouth or can’t make enough saliva, it is very important to see your doctor, as there may be an underlying health issue causing it.
Bad Breath (Halitosis)
A persistent, unpleasant odor in exhaled breath can be another red flag for an underlying health condition. While it is often caused by the foods we eat, it can also be associated with dry mouth, gastrointestinal problems, liver, kidney disease, sinus infection and chronic lung infections.
Pale Gums
Healthy gums are normally pink in color. Pale gums may be a sign of anemia, a condition where there aren’t enough healthy red blood cells in the body. Since red blood cells are responsible for carrying oxygen in the body, when the gum tissue doesn’t get enough oxygen, it may turn pale.
Irritated Red Gums
We all know the importance of flossing every day to help remove plaque. If plaque isn’t brushed and flossed away, it may harden and build up with pathogenic bacteria causing the gums to become inflamed. You may notice that the gums easily bleed during tooth brushing. Bleeding gums are not a sign of health, don’t accept this as your normal. I am sure you have heard it before, but flossing and/or interdental cleaning every day as a part of your oral care routine is not optional, it is essential.
With that said, irritated or inflamed gums may be caused by hormone fluctuations at different times in a woman’s life or certain underlying health issues. So, while many people often overlook cases of mild gum irritation, it is very important to have these checked by a medical professional.
Gum Inflammation
What may start as mild gum irritation can evolve into a serious irreversible damage to your gums and teeth if left untreated. In the early stages, pathogenic plaque and the host response may cause the gums to become inflamed, as it progresses, this may lead to receding gums and other dental problems.
Along with the physical damage to the gums and teeth, there may be microbial imbalances in the mouth that allow bacteria to enter the bloodstream and affect other areas of the body.
It is important to note, that many gums problems can be prevented with proper oral care and early diagnosis of systemic diseases. So, do not wait for the more serious irreversible symptoms to occur. Have your gums routinely checked.
Signs of gingivitis (reversible gum inflammation) include:
- Swollen, red puffy, bleeding gums
- Bad breath
- Receding gums
- Tender gums
Sign of Periodontitis (irreversible damage to soft tissue and bone, chronic inflammation) include:
- Swollen, red puffy, bleeding gums
- Receding gums
- Formation of pockets (space between teeth and gums)
- Bad breath
- Mobility and/or eventually tooth loss
- Usually not painful
- Tartar or plaque buildup
- Changes in position of teeth sometimes
The prevalence of periodontal disease is at epidemic proportions!
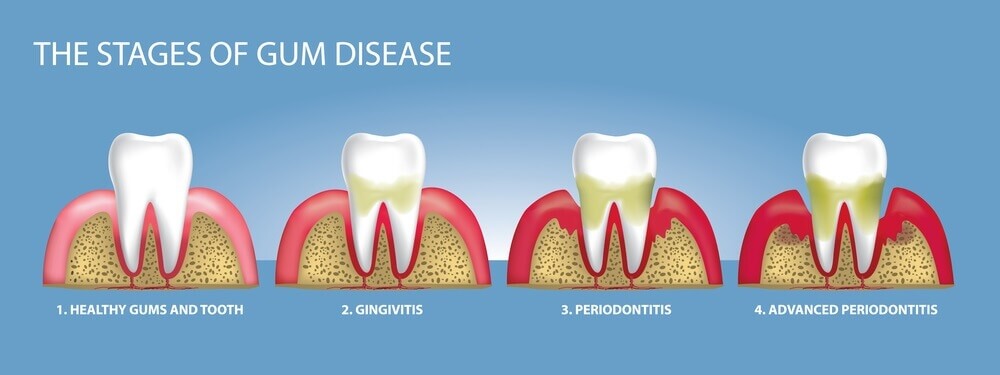
The National Health and Nutrition Examination Survey (NHANES) study conducted in 2009-2012, suggests that 46% of US adults had periodontitis. This is 64.7 million Americans![2]
That statistic does not include those affected by gingivitis which is closer to 93.9% according to a paper published in 2010 by the Journal of Dental Research.[3]
The Tongue, a Mirror to Our Digestive Health

Did you know that the appearance of your tongue can reveal a glimpse into your digestive health? A healthy tongue has a pink color with or without a thin whitish coating and small papillae, the nodules on the tongues’ surface that help us taste.
If you notice any changes in the color or appearance of your tongue, such as lumps, bumps, swelling that do not resolve within two weeks, have them checked by a dental health professional as these may be caused by an underlying health condition.
Here are a few examples of some of the more common warning signs you may see in the tongue, with their potential causes:
White Tongue
- Oral Thrush: White coated tongue or white spots may be a sign of oral thrush, a yeast infection in the mouth caused by the overgrowth of candida albicans. Candida infections may also affect other areas of the body. Infants, the elderly (especially denture wearers), those with compromised immune systems, recent antibiotic use, and diabetes are some of the main risk factors.
- Leukoplakia: White patches on tongue and mucosal tissue may appear when cells in the mouth grow excessively. A common cause is tobacco products, also called smoker’s keratosis. This condition can be brought on by repeated trauma such as ill-fitting dentures that keep rubbing and aggravating the mouth. Leukoplakia increases your risk of oral cancer.
- Oral lichen planus: White lacy or spider web like appearance on the tongue and inside of the checks. This condition may or may not have pain associated with it. It is self-limiting and does resolve on its own. Stress is thought to be a causative factor.
Red Tongue
Potential causes of red tongue may include:
- B vitamins deficiency, which can be remedied by supplementation
- Extremely red and cracked tongue as a result of a dry mouth
- Geographic tongue: a harmless condition characterized by red patches surrounded by white borders, usually on the top and sides of the tongue. May or may not cause discomfort.
- Scarlet fever: strawberry-like, red and bumpy appearance on the tongue. May be associated with strep infection and high fever. Medical attention is required.
Black Tongue
Poor oral hygiene practice may lead to a black colored tongue. The papilla may elongate and have a hair like appearance, referred to as, black hairy tongue. Certain medication, excessive coffee/tea drinking, tobacco use, antibiotics, chemotherapy, radiation to head/neck area or diabetes may also be a cause of this condition.
The Role of Diet on Oral Health

A diet high in caffeine, sugar, highly processed, and inflammatory foods such as; dairy and gluten found in grains can be detrimental to the gut and mouth. While brushing and interdental cleaning between teeth are helpful, your diet has the biggest influence on the quality of bacteria in your oral and gut microbiome. Nutritional deficiencies may also affect oral health. Remember, your teeth and gums are living tissues that need ongoing nourishment just like any other tissue in your body.
So, for optimal oral health, you need to avoid the foods that can damage your health and provide your body the necessary nutrients it needs to thrive.
In functional medicine, we often tailor the diet to the patient’s unique needs and preferences. In the context of our discussion for optimal oral care, here are some of the key foods to eat and avoid:
Foods to Limit
- Processed foods
- Sugars
- Inflammatory foods such as gluten, dairy, corn (if you like to eat bread, look for gluten free or sourdough)
- Artificial sweeteners
- MSG
- Refined vegetable oils
- Processed meats
- Alcohol
- High sugar fruits.
Foods to Eat for Better Oral Health
To avoid pesticides and chemicals commonly found in sprayed foods, try to eat organic as much as possible.
- Vegetables & greens: such as kale, spinach and broccoli
- Omega-3s rich foods such as wild salmon and tuna
- Healthy fats from avocado, coconut oil, olive oil, ghee, soaked nuts and seeds.
- Natural spices.
Vitamins & Minerals for Oral Health
Below is a list of the key vitamins and mineral for oral health, along with some of the best food sources of each. Keep in mind that in some cases, supplementation may be necessary, so always work with your doctor to test your levels.
- Vitamin A:
Egg yolks and cod liver oil.
Plant based options such as carrots and dark leafy greens are high in beta carotene, which is a precursor of vitamin A.
Not all people, however, can effectively convert beta carotene to vitamin A, so it is important to get a combination of plant and animal sources. - Vitamin D:
Very common deficiency in North America.
Produced by the body after exposure to sunshine. Also found in fatty fish like sardines, mackerel, and salmon. - Vitamin K2:
Grass fed dairy-animal fats and poultry liver.
Vitamin D3 and K2 work together to deposit calcium and other essential minerals into bones and teeth and are both needed for proper calcium absorption. - Vitamin C:
Citrus fruits, broccoli, dark leafy greens - Magnesium:
Dark leafy greens, nuts and seeds like pumpkin seeds (soak to eliminate phytates), avocados - Iodine:
Seaweed, fish, cranberries - Calcium:
Yogurt, cheese, sardines.
If you are sensitive to dairy, plant-based options that are high in calcium include leafy greens such as collard greens, arugula, kale, poppy and sesame seeds, almonds, white beans, edamame and tofu. - Zinc:
Red meat, like beef and lamb. Seafood (especially oysters), organ meats, and pumpkin seeds.
Oral Care Tips

Good oral wellness can be maintained by simple steps that only take a few minutes every day. Coupled with routine checkups and regular dental cleaning, these small daily activities can have a profound impact on your oral health and, as we have discussed, your overall health.
Below are some of the key steps to include/watch for in your daily oral care routine:
- Brush twice daily with a SOFT toothbrush. Ideally, brush first thing in the morning and last thing before bed. Confirm with your dental hygienist that your technique is right. Avoid aggressive brushing. Countless studies proclaim electric toothbrushes disrupt more plaque and food debris on and between teeth than manual brushes. Two that I like are Sonicare and Oral B Electric. Burst is also a new electric toothbrush on the scene.
- Unlike what you may have heard, use non-fluoridated toothpaste. Fluoride is a neurotoxin. A very small pea size amount of coconut oil and baking soda can be used as a replacement to toothpaste. Wetting the bristles of the brush with just water is also sufficient to remove plaque. Alternatives to fluoride-toothpaste products are available over the counter and are manufactured by varies companies. Avoid common toothpaste ingredients such as; Sodium Lauryl Sulfate, Glycerin, Triclosan, Blue & Red Dyes, Artificial Sweeteners etc. Each of these ingredients is harmful to your health.
- Interdental cleaning: floss and/or brush with interproximal brushes. Two popular types of brushes are called Soft-Picks and Proxabrush.
- Brush your tongue morning and evening.
- Avoid harsh antimicrobial rinses: Just like our gut, which hosts good and bad bacteria, not all the bacteria found in our mouth are bad. Many antibacterial mouth rinse products can actually kill ALL the bacteria in our mouth causing unhealthy problems.
Coconut oil can be used occasionally as a natural antimicrobial, antiviral, antifungal mouth rinse. It’s called oil pulling and it won’t wipe out your mouth’s ecosystem. Always spit the oil in a garbage can, not the sink or toilet as it can clog plumbing. Make sure not to use coconut oil on a regular basis as it could kill off beneficial bacteria. In addition, ongoing use can loosen up restorative cement for crowns/bridges, so speak with your dentist if that’s a concern.
A note about fluoride and mercury: both are toxic heavy metals. There are much healthier alternatives available. Silver fillings release mercury into your body which can cause adverse health issues. Consider seeing a biologic/holistic/functional medicine dentist with a fluoride and mercury-free practice and who has established protocols for the safe removal of mercury and uses biological safe restorative materials.
Final Thoughts: The Pillars of Oral & Overall Health
Poor oral health can cause disease in our body; good oral care, on the other hand, can protect us and promote optimal health and wellness.
Oral care may not always get enough attention when it comes to our overall health, although by now, we have enough evidence to know that these are deeply connected. A healthy lifestyle that focuses on nutrient dense real food, fun & efficient movement, restorative sleep, and daily stress management should always be considered our gatekeepers for ideal wellness, and the first step in optimal digestion, which begins in our mouth!
I highly recommend working with a functional dentist, who much like a functional medicine doctor, looks at the body as a whole and understands the mouth/body connection, recognizes the role diet/nutrition play in health and stays away from toxic products and procedures that unfortunately are still common in dentistry.
Oral health results in longevity and most importantly, quality of life. A great dental team who meets your needs has the potential to impact not just your mouth, but your entire well-being.



Good oral health is really important for everyone. Most people use a normal toothbrush, but there is something more important than that. If we have any oral problems or not, we need to follow our dentist’s instructions. Thanks for this information it will help so many people.