 |
Bojana Jankovic Weatherly, MD FACP MSc IFMCP Functional Medicine Doctor Gut Health Expert |
IBS | SIBO | Leaky Gut | Low FODMAPs Diet | References
In our last article, we talked about how stress can negatively affect your gut health. While chronic stress is a risk factor for gut disorders, including gastroesophageal reflux, inflammatory bowel disease and irritable bowel syndrome, it is often overlooked.[1]
What happens in many cases is that we get used to living with digestive discomfort, and as a result, we make choices to simply deal with some of the symptoms without giving them much attention. For example, you may decide not to go to the beach due to bloating, or to skip a social event because you have had diarrhea or excess gas.
But your life does not need to be controlled by your digestion.
I have seen how devastating digestive issues can be and how drastically they can impact a person’s quality of life. I believe that becoming aware of the early signs and triggers, can improve and speed up the diagnostic process and increase the likelihood of effective treatment.
In this review, I will go over three common digestive issues that are often undiagnosed or take a long time to be diagnosed. If you have the symptoms described below, talk to your qualified health practitioner.
Irritable Bowel Syndrome (IBS)

Irritable bowel syndrome is one of the most common gastrointestinal disorders that affects millions of Americans. Depending on the diagnostic criteria used, it is estimated that at least 12% of the general population may suffer from IBS. That’s over 39 million people in America alone![2]
IBS Symptoms
With IBS, the gastrointestinal tract doesn’t function normally. People with IBS experience abnormal contractions of the intestinal muscles and signals from nerves. As a result, common symptoms may include abdominal pain, bloating, changes in bowel movements, constipation or diarrhea.
Due to the severity of the symptoms in some people, IBS can prevent them for participating in everyday activities.[3]
Diagnosis:
Rome IV criteria is a diagnostic tool used by doctors to diagnose IBS. The diagnostic criteria includes recurrent abdominal pain at least one day per week for three months. The pain is associated with at least 2 of the following:
- Pain is related to having a bowel movement
- Associated with a change in frequency of the stool
- Associated with a change in the appearance of the stool.[4]
Although these criteria are present, IBS can be difficult to diagnose because there is a lack of definitive testing methods. It is usually the diagnosis of exclusion. It is recognized that food poisoning is the leading cause of IBS. Additionally, many IBS symptoms can be caused by or linked to other digestive problems. It is therefore important to be evaluated by a qualified health care professional to rule out other causes of your symptoms, as similar symptoms can occur due serious conditions such as an infection, inflammatory bowel disease, Celiac disease, or colon cancer.
For individuals with IBS with diarrhea, a new test is available for biomarkers of IBS. It is called IBS-Smart and it is a blood test developed by Dr. Mark Pimentel, a gastroenterologist and researcher.
Treatment:
Treatment for IBS may vary from one person to another depending on the underlying cause, but it typically includes a combination of dietary and lifestyle changes. It may also include medications and/or supplements that support gut motility and normal bowel movements, as well as help relax the smooth muscles of the digestive tract.
The diet for IBS focuses on identifying and eliminating food sensitivities or foods that trigger specific symptoms. It also involves encouraging the intake of foods that can promote gut health. The low FODMAPs diet has been used successfully in IBS.
Stress management activities that support the mind-body connection such as Mindfulness-Based Stress Reduction (MBSR) and yoga have been shown to improve the quality of life of IBS patients and decrease the severity of symptoms.[5,6] Similarly, gut directed hypnotherapy has been shown to be promising in alleviating symptoms of IBS and the psychological burden.[7] Acupuncture is another modality that has been found to be effective at alleviating IBS symptoms.
Small Intestinal Bacterial Overgrowth (SIBO)
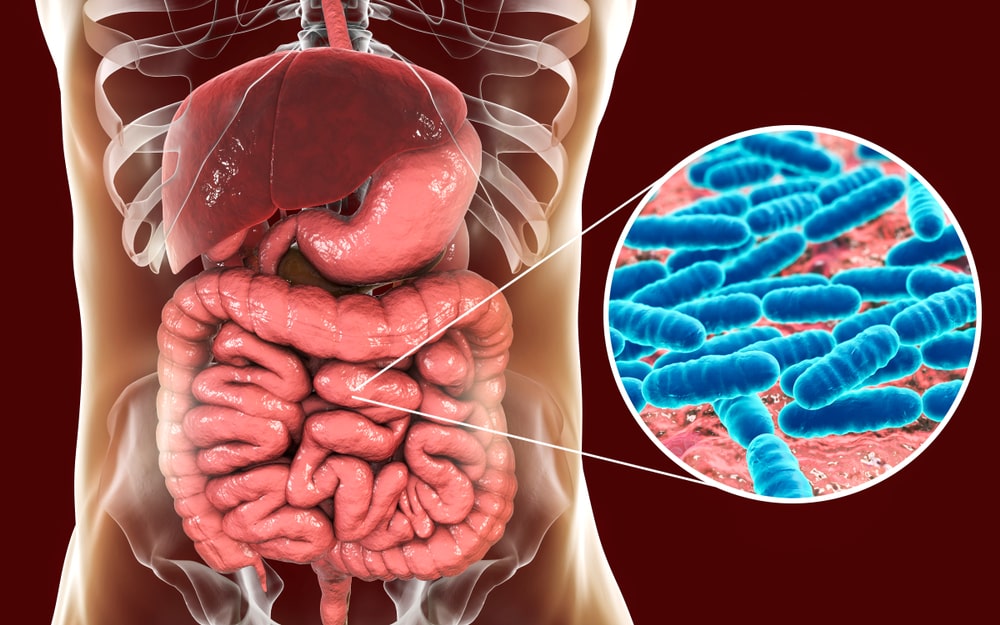
SIBO is defined as the presence of excessive bacteria in the small intestine.[8]
SIBO Symptoms:
Individuals who have SIBO have excess gas in their intestines. You may wonder how and why is this excess gas is generated. To answer that question, we need to talk about the bacteria in the gut. Bacteria eat through a process called fermentation. The result of fermentation is gas production in the intestine.
In SIBO, bacteria in the gut can overgrow due to risk factors such as compromised gut motility, anatomical abnormalities, reduction in stomach acid, pancreatic insufficiency, or immune system compromise. Overgrowth of bacteria in the small intestine can cause food to ferment before it is effectively broken down. As a result, more gas is produced, leading to symptoms such as bloating, abdominal discomfort, diarrhea or constipation, and nausea. SIBO may compromise the absorption of nutrients through the small intestine, which overtime, can lead to fatigue and nutrient deficiencies, such as B12 and iron deficiencies.[9]
Diagnosis:
The most common way to test for SIBO is a breath test that involves ingestion of lactulose or glucose and detects levels of hydrogen and methane over a 3 hour period (hydrogen and methane are bacterial by-products of fermentation of carbohydrates and polyols). Since SIBO can be similar to other digestive problems, your doctor may order additional tests, including a test for Celiac Disease, or a stool test to check for bacteria and parasites, or food sensitivities.
Treatment:
The treatment for SIBO may vary from one individual to another. One common nutritional recommendation for individuals who have SIBO, which can also be effective for IBS, is a low FODMAPs diet.
Low FODMAPs Diet

FODMAPs stand for Fermentable Oligo-, Di- and Mono-saccharides And Polyols. These are short-chain carbohydrates that are the main food source of small intestinal bacteria. By eliminating high FODMAP foods, you “starve” and decrease the number of bacteria in the small intestine.
Sticking to a low FODMAPs diet, however, can be quite restrictive, as you eliminate a wide range of foods. While you may start by eliminating gluten, dairy, certain fruits such as figs and mangoes, and most sweeteners, your doctor may also recommend eliminating other foods you may be sensitive to.
Depending on your current situation, additional lifestyle changes and medications may be recommended. If your doctor recommends a low FODMAPs diet, do not be discouraged! This is not intended to be a “forever” diet. You should discuss with your doctor and dietitian or nutritionist, when and how a slow re-introduction of foods that are not low in FODMAPs should begin. This is an excellent resource for variations on diets that can help individuals with SIBO.
SIBO treatment typically includes antibiotics, or antimicrobial herbs, which are less studied but have been shown to be effective at treating SIBO.[10] Be sure to consult with a qualified healthcare provider before altering your diet or starting any new supplements or medications.
In my clinical experience, there is no one-size-fits-all approach with respect to dietary recommendations and treatment. It is always important to consider triggers, irritants, and other factors affecting an individual with SIBO or IBS, which is why it is imperative to work with a qualified healthcare provider.
Leaky Gut (Increased Intestinal Permeability)
To better understand what leaky gut is, let me describe a “normal” gut. Your intestinal walls are naturally semi-permeable to allow micronutrients to get into your bloodstream, but just permeable enough to prevent harmful substances and toxins from passing through.
With leaky gut, intestinal permeability increases, allowing bacteria, their products and toxins to “leak” into your bloodstream. As a result, your immune system will recognize these as foreign invaders and attack them, leading to increased inflammation and potentially increased risk of autoimmunity.[11]
Leaky Gut Symptoms:
Consequences of leaky gut can include inflammation and autoimmune disease. Small intestinal bacterial overgrowth can lead to leaky gut. Inflammatory bowel disease and Celiac disease have also been associated with increased intestinal permeability.
Diagnosis:
Diagnosis and treatment of leaky gut are current areas of active research. The diagnosis for increased intestinal permeability is usually based on an evaluation of your medical history, current symptoms, and risk factors. Multiple food sensitivities can also be a sign of increased intestinal permeability. Increased intestinal permeability is often overlooked and is an important area of research.[12,13,14]
While zonulin increase has been correlated with leaky gut, it is not a reliable marker of it.[15]
Treatment:
Depending on the underlying cause, different treatment approaches may be required. Just like IBS and SIBO, diet and lifestyle play key roles. Specific to leaky gut, a diet plan that focuses on eliminating inflammatory, processed foods, eliminating food additives and pesticides, and consuming gut-healing, whole foods is key. More research in this area is needed to elucidate the optimal management.
Due to increased intestinal permeability, people with leaky gut can have multiple food sensitivities. While most diets for leaky gut start by eliminating foods known to irritate the gut such as gluten, certain grains, processed foods, and dairy, additional dietary changes may be needed to account for individual sensitives. It is also important to note that restrictive elimination diets are not “forever” diets and can result in nutrient deficiencies. It is important to work with a qualified healthcare provider to determine whether it is advised that you follow a particular elimination diet, for how long and how to re-introduce the foods.
Final Thoughts
These three common digestive conditions can all drastically affect one’s quality of life. Unfortunately, they can often be overlooked or misdiagnosed.
These conditions rarely develop overnight. They may be triggered by a gastrointestinal infection. They may start with occasional digestive symptoms such as gas, bloating, and constipation. Eventually, many people are surprised or relieved to learn they have a medical condition after a long and frustrating journey with their symptoms.
Finding an experienced healthcare provider is particularly important since a major part of the treatment for SIBO, IBS and leaky gut includes specific dietary protocols that can be restrictive in nature and not easy to do. These often have a customization component, where the diet has to be tailored to each individual to address individual food sensitivities. While on a restrictive diet, it is important to ensure that one does not develop a nutrient deficiency. A plan to prevent this should be discussed with a qualified healthcare professional ahead of time. Reintroducing foods after an elimination diet is another important component of the plan that should be discussed with a qualified physician, dietitian or nutritionist.
Becoming aware and recognizing some of the common warning signs, connecting them with the relevant risk factors, and taking the right actions are key. A qualified healthcare provider can help you find the correct diagnosis and the most effective treatment based on your individual needs.
References
- http://www.jpp.krakow.pl/journal/archive/12_11/pdf/591_12_11_article.pdf
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4476871/
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5625880/
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5704116/
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4438173/
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6178327/
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6274728/
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3099351/
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2890937/
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4030608/
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5440529/
- https://www.ncbi.nlm.nih.gov/pubmed/28950279
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4451427/
- https://www.ncbi.nlm.nih.gov/pubmed/22731712/
- https://www.sciencedirect.com/science/article/pii/S2352551717300288
Nothing stated in this article is intended or should be taken to be the practice of medical or counseling care. The information made available in this article, is strictly for informational and entertainment purposes only. The information in this article is NOT (and should not be used as) a substitute for professional psychiatry, psychology, medical, nursing, or professional healthcare advice or services, nor is it designed to suggest any specific diagnosis or treatment. Please always seek medical advice from your physician or a qualified health care provider regarding any medical questions, conditions or treatment, before making any changes to your health care regimen, medications or lifestyle habits. None of the information in this article is a representation or warranty that any particular drug or treatment is safe, appropriate or effective for you, or that any particular healthcare provider is appropriate for you. Never disregard professional medical advice or delay seeking help from a health care provider due to something you have read, heard or seen in this article. Your use of the information in this article does not create in any way a physician-patient relationship, any sort of confidential, fiduciary or professional relationship, or any other special relationship that would give rise to any duties. This article does not recommend or endorse any specific tests, healthcare providers, procedures, or treatments, and if you rely on any of the information provided by this article, you do so solely at your own risk.

